Electrocardiogram of an 85 year-old man with hypertension, hyperlipidemia, coronary artery disease, CABG 12 years earlier who presented to the ER with prolonged ischemic chest pain.
Rate 75/min
PR 0.19 sec
QRS 0.08 sec
QT 0.36 sec
QTc 0.40 sec
QRS axis –65ş
Interpretation: Abnormal ECG. Sinus rhythm. Borderline left atrial abnormality. Left axis deviation. Left anterior fascicular block. Hyperacute ST segment elevation in the antero-lateral precordial leads.
The patient was diagnosed with an acute myocardial infarction and started on thrombolytic agent (rPN) by the ER Physician. Within 15 mins the patient became hypotensive, developed elevated JVP and pansystolic murmur grade 3/6 at the left sternal border radiating to the right side of the sternum.
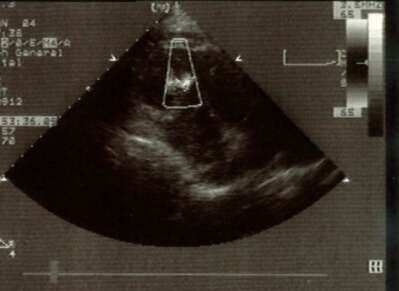
Clinical diagnosis of the acute ventricular septal rupture was confirmed by an emergent echocardiogram (panel below) which showed akinesis of the anterior wall and septum and abnormal flow across the distal part of the ventricular septum directed from left-to-right.
In view of hemodynamic instability, previous CABG and senility the patient was not accepted for cardiovascular intervention. Developed progressive cardiogenic shock not responding to medical therapy and expired.
<< back to ECG Decoder